Designing Back Exercise: from Rehabilitation to Enhancing Performance
Stuart McGill, Ph.D. Professor of Spine Biomechanics,
Faculty of Applied Health Sciences, Department of Kinesiology, University of Waterloo
(Download PDF, 260Kb)
Many have asked me to write a short overview to assist increasing the competency of clinicians. But after writing two textbooks based on our hundreds of scientific publications, I feel as though I have already said what is necessary and important in a cohesive story. Here are few thoughts for exercise professionals who deal with issues related to the assessment and design of therapeutic exercise for the back, to assist them in becoming elite professionals. Many clinicians follow a “recipe” for assessment, treatment or performance training. Using this generic approach ensures “average” results – some patients/clients will improve and get better, but many will fail simply because the approach was above or below the optimum level necessary to address the deficit. The program and approach introduced here will help you to become an elite corrective exercise and training specialist. Invest the effort to enhance your knowledge and techniques and you will have success where others have failed. Many times, we have had a breakthrough with an influential client – be they a pro athlete or business person. Subsequently they become your best referral service.
The cause (and elimination of it)
The first step in any exercise progression is to remove the cause of the pain, namely the perturbed motion and motor patterns. For example, the flexion intolerant back is very common in todays society. Giving this type of client stretches such as pulling the knees to the chest may give the perception of relief (via the stimulation of erector spinae muscle stretch receptors) but this approach only guarantees more pain and stiffness the following day as the underlying tissues sustain more cumulative damage. Eliminating spine flexion, particularly in the morning when the discs are swollen from the osmotic superhydration of the disc that occurs with bedrest, has been proven very effective with this type of patient. Realize that the spine discs only have so many numbers of bends before they damage. Keep the bends for essential tasks such as tying shoes rather than using them up in abdominal training. Many lifestyle and occupational examples are provided in the textbook “Low back disorders: Evidence based prevention and rehabilitation” to guide the elimination of the cause of a clients back troubles – the clinician will find that half of Resources: McGill, S.M. (2007) Low back disorders: Evidence based prevention and rehabilitation, Second Edition, Human Kinetics Publishers, Champaign, IL, U.S.A. McGill, S.M. (2007) (DVD) The Ultimate Back: Assessment and therapeutic execise, www.backfitpro.com McGill, S.M. (2009) Ultimate back fitness and performance – Fourth Edition, Backfitpro Inc. Waterloo, Canada (www.backfitpro.com). 2 their initial effectiveness will be due to preventing the cause (ie, a flawed movement pattern)! This need not be so complicated. Consider the client who stands slouched where the back muscles are chronically contracted to the point of chronic muscle pain. The family doc typically prescribes muscle relaxants which fail to work. The clinician addresses the postural cause and corrects standing to shut the muscles off and remove the associated crushing load from the spine. The client exclaims, “You’re magical – you just took the ache out of my back”.
Building the scientific foundation:
Myths and controversies regarding spine function and injury mechanisms are common. Consider “the cause” of back troubles, specifically the common perception regarding common injury pathways in which the back is hurt in an “event”. Generally statistics are compiled from epidemiological approaches which ignore the large role of cumulative trauma. Compensation board data is often used however, and they ask clinicians to fill out reports and name the “event” that caused the “injury”. For example, “Mr X lifted and twisted” at the time that the injury occurred. Kinesiologists and clinicians know that twisting is different from generating twisting torque, but very few of the individuals filling out the reports will know. So, was it twisting torque? Or, was it being twisted, that caused the injury? Further, despite the injury reporting system geared to the reporting of the “event” associated with the “injury”, very few back injuries occur this way. Evidence of the process of disc herniation provides a proof of principle. For example the damaging mechanism leading to herniation, or prolapse, is repeated lumbar flexion requiring only very modest concomitant compressive loads (Callaghan and McGill, 2001). This trauma accumulates with little indication to the future patient. With repeated flexion cycles the annulus breaches layer by layer with progressive delamination of the layers (Tampier et al 2007). This allows gradual accumulation of nucleus material between the delaminated layers. The location of the annulus breaches can be predicted by the direction of the bend. Specifically, a left posterior-lateral disc bulge will result if the spine is flexed with some additional right lateral bend (Aultman et al, 2004). Subsequent twisting leads circumferential rents in the annulus that tends to make McKenzie extension approaches for these clients useless, or even exacerbating (Marshall and McGill, 2010). This is critical information for the clinician, both in terms of prevention and in treatment. Avoiding this specific directional cause will lead to optimal therapeutic exercise design together with elimination of activities in the patient’s daily routine identified as replicating the cause.
Many therapy approaches have the objectives of strengthening muscle and increasing spine range of motion. This is problematic (Parks et al, 2003) since those who have more motion in their backs have a greater risk of having future back troubles. Strength may, or may not, help a particular individual as strength without control and endurance to repeatedly execute perfect form increases risk. Interestingly, the differences between many “troubled backs” (the chronic back with recurrent episodes) and matched asymptomatic controls performing the same jobs have been shown to be variables other than strength or mobility. Rather deficits in motion and motor patterns have been documented as being more critical and thus should be targets for therapeutic exercise. For example, people with troubled backs use their backs more. Generally, they walk, sit, stand and lift using mechanics that increase back loads. Many of them have stronger backs but are less endurable than matched asymptomatic controls (McGill et al, 2003). They tend to have more motion in their backs and less motion and load in their hips. A common aberrant motor pattern is known as “gluteal amnesia” (McGill, 2007) which may be both a 3 common consequence of back troubles and probably a cause of them as well. Obviously for this category of client, exercises to enhance the integration of the gluteal muscles will help their backs, and also their knees. Optimal back exercise therapy results from the identification of these patients with perturbed patterns followed by specific corrective exercise – this precedes all other exercise therapy.
The science of spine stability: Effective spine stabilization approaches must begin with a solid understanding of what stability is. From a spine perspective it has little to do with the ability to balance on a gym ball. This is simply the ability to maintain the body in balance which is important but does not address the unstable spine. In fact, in many instances the unstable spine is also flexion intolerant and with associated intolerance to compression. Sitting on an exercise ball performing movement exercises increases spine compression to a flexed spine. This retards progress – it is generally a poor choice of back pain exercise until quite late in a therapeutic progression. True spine stability is achieved with a “balanced” stiffening from the entire musculature including the rectus abdominis and the abdominal wall, quadratus lumborum, latissimus dorsi and the back extensors of longissimus, ilioicostalis and multifidus. Focusing on a single muscle generally does not enhance stability but creates patterns that when quantified result in less stability. It is impossible to train muscles such as transverse abdominis or multifidus in isolation – people cannot activate just these muscles. Do not perform abdominal hollowing techniques as it reduces the potential energy of the column causing it to fail at lower applied loads (McGill, 2009). Interestingly a recent clinical trial (Koumantakis et al, 2005) compared the efficacy of many of the exercises that I quantified and published in Physical Therapy (McGill 1998), with the same exercises combined with specific transverse abdominis isolation (hollowing etc.). Adding the specific transverse abdominis training reduced efficacy! Instead, the abdominal brace (contracting all abdominal muscles) enhances stability. Target contraction levels for bracing and training techniques are described in McGill (2006). Finally, some provocative tests, such as a shear test, will help reveal which classification of patient is best suited for a stabilization approach (Hicks et al, 2005).
Tolerance and Capacity: Determining the tolerance and capacity of each individual is paramount to ensure that a given exercise dosage is matched to the client. Each individual has a loading tolerance which, when exceeded, will cause pain and ultimately tissue damage. For example, a patient may tolerate a birddog extension posture but not a superman extension over a gym ball which imposes twice the compressive load on the lumbar spine. A person’s capacity is the cumulative work that he or she can perform before pain or troubles begin. An example, someone who can only walk 20 meters before pain sets in has a low capacity. This kind of person won’t benefit from therapeutic exercise that’s performed 3 times per week; instead, he or she has a better chance with 3 sessions per day. Corrected walking in 3 short sessions per day, never exceeding the current tolerance and capacity, is an alternate approach to building capacity. Typically, patients will progress to 1 session per day as their pain-free capacity grows and then be tolerant of a good session with their clinicians.
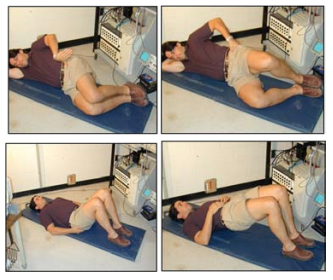
Interpreting client presentation: Our approach to client assessment incorporates a strong biomechanical foundation, and blends expertise from various disciplines. First, an impression is formed from the first meeting of the client – their sitting posture, how they rise from the chair, their initial gait pattern etc (see figure 1). Then a history is taken looking for possible candidate injury mechanisms, and perceived pain exacerbators and relievers. Observation continues during some basic motion patterns as the evaluation process proceeds delving further into the mechanics and nature of the symptoms. Then provocative tests are performed to identify motion and motor patterns that are tolerated.
Interpreting client presentation
Specific exercise programs for a client with back pain are derived from the following process (It is assumed that appropriate medical screening has transpired):
- Observe everything, starting with the client rising from a chair.
- History – link injury mechanisms, pain mechanisms with specific activities and past exercise regimens. Of course if
sinister “red flags” appear make the appropriate referral.- Perform provocative tests – what loads, postures and motions exacerbate, what relieves?
- Perform functional screens and tests – Are there perturbed postural, motion and motor patterns?
- If the clinical picture is complex and beyond your comfort zone, develop a referral relationship with a competent corrective exercise specialist. This is reciprocal and will serve you well with more clients in the future
Specifically we include a range of motions, postures, and loads. All information is used to formulate the plan for corrective exercise and the starting dosage of tolerable therapeutic exercise. The process concludes with functional screens and tests that were chosen based on information obtained in the preceding process (the assessment process is well documented in McGill, 2007). These results are used to substantiate some speculation as to the existence of perturbed motion and motor patterns and for considering exercise choice and rates of subsequent exercise progression.
Figure 1: Poor standing posture causes constant spine load and chronic contracture of the erector spinae muscles causing muscular pain (A). Rising from a chair with dominant hamstrings because of pain inhibiting the gluteal muscles causes higher back loads (B).
Example of some provocative tests that are helpful
Provocative testing is a potent tool in the assessment of back problems, and is easily performed. I have tried to illustrate a wide variety of these, together with some corrective techniques in a DVD (see McGill, 2007). See Figure 2 for an example of provocative testing for compressive load tolerance. This posture-modulated tolerance test provides powerful information and can serve as a guide to avoid damaging/exacerbating activity, and it also helps to design appropriate therapy.
Figure 2: An example of provocative testing. The patient compresses the spine by grabbing the side edges of the seat and pulling down. When doing this with an upright back (a), the torso is stiffened with muscle activity. The test is then repeated in a slouched posture (b); discomfort in this position as compared to an upright back shows a lower tolerance when the spine is flexed (and a flexion intolerant patient). This reveals where the spine tolerance is highest, and therefore a posture to begin therapeutic exercise.
More practical information can be gleaned from simply asking whether a client has better and worse days. Even though it seems straightforward, it can’t be stressed enough that if there are indeed better and worse days, it means that some activities help and others hurt. Find out what they are and eliminate the exacerbating elements. For example, if sitting isn’t tolerated, avoidance of flexion by using a lumbar support will help, together with organizing tasks to eliminate prolonged sitting. This is known as “spine hygiene” and will build more capacity for the client to work with you. Your efforts here will be well rewarded with more success. Specific exercises designed to combat the cumulative stresses of sitting are then prescribed.
Reducing the risk of injury:
No exercise professional can be fully successful without removing the movement flaws that cause of back troubles in patients throughout the day. Controversial recommendations such as “when lifting, bend the knees and keep the back straight” rarely address the real issue, despite their popularity. Few patients are able to use this strategy in their jobs and furthermore, this is often not the best strategy. For example, the “golfers lift” is much more joint conserving for repeated lifting of light loads from the floor. Another example illustrates the poor choice of movement strategies for a particular task. For example observe the client who transitions to laying on the floor by using a deep squat – this overloads their back. Squatting is appropriate for getting off a toilet or chair but not for dropping to the floor. Instead a lunge that does not bend the spinal discs is a much more appropriate choice. Again, this builds capacity for them to accomplish more in their training session with you (see McGill, 2007 for full explanation and evidence for spine sparing guidelines).
Linking Anatomy with Function:
Consider the usual and popular approach to train the abdominal wall muscles by performing situps or curl-ups over a gym ball for example. But consider the rectus abdominis where the contractile components are interrupted with transverse tendons giving the “six pack” look. The muscle is not designed for optimal length change but rather to function as a spring. Why have these transverse tendons in rectus abdominis? The reason is that when the abdominals contract, “hoop stresses” are formed by the oblique muscles that would split the rectus apart. In addition to Figure 2: An example of provocative testing. The patient compresses the spine by grabbing the side edges of the seat and pulling down. When doing this with an upright back (a), the torso is stiffened with muscle activity. The test is then repeated in a slouched posture (b); discomfort in this position as compared to an upright back shows a lower tolerance when the spine is flexed (and a flexion intolerant patient). This reveals where the spine tolerance is highest, and therefore a posture to begin therapeutic exercise. 6 the spring-like architecture of the muscle consider how it is used. People rarely flex the rib cage to the pelvis shortening the rectus in sport or everyday activity. Rather they stiffen the wall and load the hips or shoulders – if this is performed rapidly such as in a throw or movement direction change, the rectus functions as an elastic storage and recovery device. When lifting weights it stiffens to efficiently transmit the power generated at the hips through the torso. Those individuals who do actively flex the torso (think of cricket bowlers and gymnasts) are the ones who suffer with high rates of disc damage and pain.
Figure 3: Curlup over a gymball motions stresses the discs and unwisely uses capacity (a) while the `Stir the pot` exercise spares the painful discs of motion and builds abdominal athleticism (b).
Now revisit the common training approach of curling the torso over a gym ball that replicates the injury mechanics while not creating the athleticism that enhances performance. This is a rather poor choice of exercise for most situations. Yet many clients will expect that a gymball be used. Play a trick on these clients and retain the gymball but change the exercise from a spine breaking curlup to a plank where the elbows are placed on the ball. Now “stir the pot” to enhance the spring and spare the spine – this is a much superior exercise for most people. (See figure 3).
Rehabilitation Exercise – Biomechanics and Clinical Practice:
Rehabilitation is a staged process: My textbooks illustrate the many considerations and techniques to hone clinical skills at each stage (see list below):
Stages of therapeutic exercise:
- Corrective exercise
- Groove appropriate and perfect motion and motor patterns. Encode movement engrams.
- Build whole body and joint stability (mobility at some joints such as the hips and stability through the lumbar spine)
- Increase endurance And for occupational/athletic clients:
- Build strength
- Develop speed, power, agility
The first stage of designing the appropriate corrective exercise emanates from the identification of any perturbed motion and motor patterns. Every exercise is considered within the working diagnostic hypothesis such that the first time the exercise is performed, it is considered a provocation test. If it is tolerated, the client proceeds. If it is not tolerated the technique is reexamined and adjusted and/or a more tolerable variation is tried (see McGill et al, 2009, for some examples with stabilization exercise). Many examples of corrective exercise are in my books and a couple are introduced here. For example, gluteal muscle activation retraining based primarily on the original work of Professor Janda has been honed in our own lab (see figure 4). This cannot be accomplished with traditional squat training (McGill, 2007). Chronic back pain tends to cause hip extension using the hamstrings and subsequent back extension using the spine extensors creating unnecessary crushing loads. Gluteal muscle reintegration helps to unload the back. Another critical concept for this stage of exercise design is that technique “details” are important. It is not a matter of client performing an exercise – it is a matter of the client performing the exercise with perfection. Exercise form, subtle maneuvers to eliminate pain, pacing, duration, and other coconsiderations are all extremely important. The next stage in the progressive algorithm is to groove patterns to ensure stability. Stability is considered at two levels – both joint stability (in this case spine stability) and whole body stability. Quantification of stability proves that these two objectives are fundamentally different and need two different exercise approaches. Our observation is that the two types of stability are often confused in the clinic/gym.
Figure 4: Chronic back pain tends to cause people to use their hamstring muscles, instead of their gluteals to extend the hip. This changes patterns that increase spine load when squatting. Performing the back bridge, squeezing the gluteal muscles, and eliminating hamstrings helps to establish gluteal dominance during hip extension. Clinical cues are presented in McGill, 2009.
Variations of our “Big 3” stabilization exercises have been quantified and selected for their ability to ensure sufficient spine stability and optimal motor patterns, they spare the spine of many injury mechanisms and pain exacerbators, and are designed to build muscle endurance (see figures 5 and 6). Then specific muscle group endurance is enhanced. Spine stability requires that the musculature be cocontracted for substantial durations but at relatively low levels of contraction. This is an endurance and motor control challenge – not a strength challenge. For many clients wanting to accomplish tasks of daily living pain free, this is sufficient. In the preceding progressions, of course strength is enhanced as are specific patterns such as the ability to squat, push/pull, lunge etc.
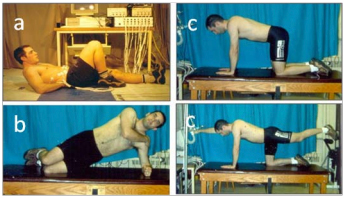
Figure 5: The “big 3” stabilizations exercises selected to create muscle patterns that ensure stability are the curl-up (a), the side-bridge (b), and the birddog (c). While we have quantified many variations and progressions, there are several cues for correct form. For example, during the curl-up, try and remove any motion from the lumbar spine, and the cervical spine. Progression included pre-bracing of the abdominal wall, elevating the elbows off the floor, breathing, to name a few. The beginner’s side-bridge is held for sets of 10 second contractions before more challenging progressions are attempted. During the birddog, making a fist and cocontracting the arm and shoulder is a progression that enhances the contraction levels in the upper erector spinae.
But strength is not specifically trained since this requires overload and elevated risk – this is reserved for performance training. Many people, whether they have athletic objectives (such as wanting to play golf) or have demanding occupations will fall into this category. On the other hand, many patients confuse health objectives (minimizing pain, developing joint sparing strategies) with performance objectives (which require risk) and compromise their progress with specific strength training too early. Many exercises typically prescribed to low back patients are done so without the clinician having knowledge of the spine load and associated muscle activation levels. For this reason, we have quantified exercises in this way (see Axler and McGill, 1997, McGill, 2002, Callaghan et al, 1998, Kavcic et al, 2004a, Kavcic et al 2004b etc) to allow evidence based decisions when planning optimal exercise progressions.

Figure 6: There are many progressions from low joint load stabilization exercises to beginners variations to stiffen and balance the anterior chain (a), and the posterior chain (b). These are examples.
Caveats for Therapeutic/corrective exercise
Keep the duration of isometric exercises under 10 seconds and build endurance with repetitions, not by increasing the duration of the holds. Near infrared spectroscopy of the muscles showed us this was the way to build endurance without the muscles cramping from oxygen starvation and acid buildup.
Use the Russian descending pyramid to design sets and reps to make bigger initial gains in progress towards a painfree back (See McGill 2009).
Maintain impeccable form to enhance available strength, and maintain the spine in its strongest (most tolerable) posture.
Training for performance: Training the back for performance (for either athletic or occupational application) requires different approaches and objectives than training to fulfill rehabilitation objectives. Some of the techniques developed in our work with world class athletes are rather extensive and are better developed in my “Ultimate back fitness” textbook within the context of valid mechanisms and evidence. These include the progressions from establishing motor control patterns once the appropriate corrective exercise was performed, through to stability, endurance, strength, speed, power and agility. A note is needed here – power development in the spine is usually very risky. Instead, power is developed about the shoulders and hips to both increase performance and to minimize risk to the spine and related tissues.
An interesting example is provided with speed training. Many train speed by using resistance exercise for strength gain. But speed usually requires superior relaxation. This apparent paradox can be exemplified this way. Consider the golf swing. The initiation of the downswing involves some muscle contraction but too much actually slows the swing. Speed comes from compliance and relaxation. At the instant just before ball contact, the farthest ball hitters in the world then undergo a full body contraction which creates a superstiffness throughout the entire linkage. Then, just as quickly the stiffening contraction is released to allow compliance and speed in the swing follow through. This same cyclic interplay between relaxation for speed and contraction for stiffness is measured in the best sprinters in the world, and the best lifters etc. So the rate of muscle contraction is only important when the muscle can be released just as quickly – only a few in the world are able to do this. These examples show why traditional strength training is usually a detriment to performance. Techniques of “superstiffness” used by strength athletes are important to understand when being mindful of the patient who may be able to grasp some of these concepts and, for the first time perhaps be able to rise from the toilet unassisted. These newest concepts are compiled and documented in my recent textbook “Ultimate Back Fitness and Performance.” (McGill, 2009).
8 Essential components of Superstiffness:
- Utilize rapid contraction, then relaxation, of muscle. Speed results from relaxation for speed but also stiffness in some body regions (eg core) to buttress the limb joints to initiate motion, or enhance impact.
- Tune the muscles. Storage and recovery of elastic energy in the muscles require optimal stiffness which is tuned by the activation level.
- Enhance muscular binding and weaving. When several muscles contract together they form a composite structure where the total stiffness is higher than the sum of the individual contributing muscles.
- Direct neuronal overflow. Strength is enhanced at one joint by contractions at other joints – martial artists call this “eliminating the softspots”.
- Eliminate energy leaks. Leaks are caused when weaker joints are forced into eccentric contraction by stronger joints.
- Get through the sticking points. The technique of “spreading the bar” during the sticking point in the bench press is an example of stiffening weaker joints.
- Optimize the passive tissue connective system. Stop inappropriate passive stretching! Turn your athletes into Kangaroos!
- Create shockwaves. Make the impossible lifts possible by initiating a shockwave with the hips that is transmitted through a stiff core to enhance lifts, throws, strikes etc.
Finally consider exercises such as the squat. Interestingly when we measure world class strongmen carrying weight, NFL footballers running planting the foot and cutting – neither of these are trained by the squat. This is because these exercises do not train the quadratus lumborum and abdominal obliques which are so necessary for these tasks. In contrast, spending less time under a bar squatting and redirecting some of this activity with asymmetric carries such as the farmers walk (or bottoms-up kettlebell carry – see figure 7) builds the athleticism needed for higher performance in these activities in a much more “spine friendly” way. The core is never a power generator as measuring the great athletes always shows that the power is generated in the hips and transmitted through the stiffened core. They use the torso muscles as anti-motion controllers, rarely motion generators (of course there are exceptions for throwers etc but the ones who create force pulses with larger deviations in spine posture are the ones who injure first). Many more progressions to enhance athleticism in a spine sparing way are provided in my text “Ultimate back fitness and performance”.
Figure 7: The asymmetric kettlebell carry challenges the lateral musculature (quadratus lumborum and oblique abdominal wall) in a way never possible with a squat. Yet this creates necessary ability for any person who runs and cuts, carries a load etc.
As I stated at the outset, I have told the full story in my books. I feel that this short paper shortchanges the reader as it simply cannot convey the components necessary to be an elite clinician, but at least it may elevate awareness of some of the issues. Those who strive to be the best will never need to be concerned about a business model. Get those difficult backs better, when your peers have failed, and clients will flock to your door. I wish you a most enjoyable journey
References
Aultman, C.D., Scannell, J., and McGill, S.M. (2005) Predicting the direction of nucleus tracking in porcine spine motion segments subjected to repetitive flexion and simultaneous lateral bend. Clinical Biomechanics, 20:126-129.
Axler, C., and McGill, S.M. (1997) Low back loads over a variety of abdominal exercises: Searching for the safest abdominal challenge. Medicine and Science in Sports and Exercise, 29(6):804-811.
Callaghan, J.P., Gunning, J.L., and McGill, S.M. (1998) Relationship between lumbar spine load and muscle activity during extensor exercises. Physical Therapy, 78(1): 8-18.
Callaghan, J.P., and McGill, S.M. (2001) Intervertebral disc herniation: Studies on a porcine model exposed to highly repetitive flexion/extension motion with compressive force. Clinical Biomechanics, 16(1): 28-37.
Hicks, G.E., Fritz, J.M., Delitto, A., and McGill, S.M. (2005) Preliminary development of a clinical prediction rule for determining which patients with low back pain will respond to a stabilization exercise program. Archives of Physical Medicine and Rehabilitation, 86(9): 1753- 1762.
Kavcic, N., Grenier, S.G., and McGill, S.M. (2004a) Determining tissue loads and spine stability while performing commonly prescribed stabilization exercises. Spine, 29(11): 1254-1265.
Kavcic, N., Grenier, S., and McGill, S. (2004b) Determining the stabilizing role of individual torso muscles during rehabilitation exercises. Spine, 29(11):1254-1265.
Koumantakis GA, Watson, PJ, Oldham, JA, Trunk muscle stabilization training plus general exercise versus general exercise only: Randomized controlled trial with patients with recurrent low back pain. Physical Therapy, 85(3):209-225.
Marshall LW and McGill SM. (2010) The role of axial torque in disc herniation. Clinical Biomechanics, 25(1):6-9.
McGill, S.M. Invited Paper. (1998) Low back exercises: Evidence for improving exercise regimens. Physical Therapy, 78(7): 754-765.
McGill, S.M. (2007) Low back disorders: Evidence based prevention and rehabilitation, Second Edition, Human Kinetics Publishers, Champaign, IL, U.S.A.
McGill, S.M., (2007) (DVD) The Ultimate Back: Assessment and therapeutic exercise, www.backfitpro.com
Click to download PDF of paper.

You may also benefit from Back Mechanic: The step-by-step McGill Method to fix back pain. This book guides you through a self-assessment of your pain triggers, then shows you how to avoid these roadblocks to recovery. Whether you’re struggling with a disc bulge, stenosis, spondylolisthesis, muscle strain, or even leg pain associated with a herniated disc, you will be able to wind down your discomfort and match your unique symptoms with the approach that is right for you.